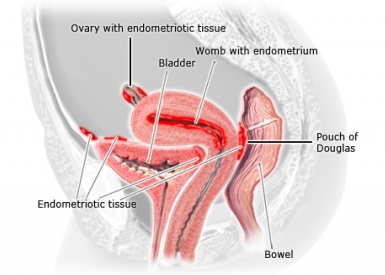
What is Endometriosis?
Endometriosis is a women’s health disorder when the endometrium, or lining of a woman’s uterus (womb), grows in other parts of the body. Although it is most common in women in their 30s and 40s, it can also occur in younger girls. Before understanding why endometriosis causes pain and problems, we should review the monthly menstrual cycle.
During the course of each cycle, the lining of a woman’s uterus builds up with blood vessels and tissue in preparation to receive the egg that gets released from one of the ovaries. If sperm does not fertilize the egg, the uterus sheds the tissue and blood. This is called menstruation, or our period.
Endometrial cells outside the uterus act similarly and respond to the female hormones that control menstruation. The endometrial tissue, regardless of where it is in the body, thickens and bleeds, except there is no exit for the secretion – they cannot be expelled through the vagina. This build up of tissue results in abnormal growths, which can cause scarring, inflammation. Over time, these growths become larger and more painful.
Endometrial cells can be found in the abdominal cavity or in the fallopian tubes, on the outside of the womb, on the ovaries, or between the womb and the rectum (called the Pouch of Douglas).
Symptoms of Endometriosis:
As mentioned earlier, many women have no idea that they could be suffering from this disorder. Because many of the symptoms occur in varying degrees of severity to many women, it can often go undetected. Interestingly, the amount of pain a woman feels does not determine whether or not she has endometriosis and it does not indicate how much endometriosis (or how many growths) she has.
Symptoms can include:
– Very painful menstrual cramps; the pain may get worse over time
– Ineffectiveness of standard, over the counter pain medication
– Chronic pain in the lower back, intestines, pelvis or abdomen
– Spotting or bleeding between menstrual periods
– Fatigue
– Pain during or after sex
– Painful bowel movements or painful urination during menstrual periods
– Diarrhea, constipation, bloating, or nausea, especially during menstrual periods
– Infertility or not being able to get pregnant
What causes endometriosis?
There is no definite known cause of endometriosis, but there are several theories. The most common is ‘retrograde menstruation’ (or transtubal migration)– when endometrial cells travel backwards, up the fallopian tubes and into the body. Another possibility is that parts of the abdominal lining turn into endometrial tissue. Since both are descended from embryonic cells, certain abdominal cells have the ability to specialize and take on the structure and function of endometrial cells. Another theory is that endometrial cells get carried to other parts of the body through the lymph system or blood system.
Additionally, new research by the Endometriosis Association shows that there are links between dioxin (TCCD) exposure and the development of endometriosis. Dioxin is a toxic chemical byproduct of pesticide manufacturing, bleached pulp and paper products, and medical and municipal waste incineration. Most ordinary tampons and pads are bleached with chlorine and as a result have been linked to having trace amounts of dioxin in them. That’ is why organic and natural chlorine free products, such as Maxim tampons, are being increasingly valued for their safety.
Risk factors for endometriosis include:
– never having given birth
– periods that last more than 7/8 days
– menstrual cycles that last less than 27 days
– a history of pelvic infection
– a health problem in which the passage of menstrual blood is obstructed
– a family member, such as a mother or sister, who has endometriosis
Treatment options:
The treatment of endometriosis depends on several factors such as age, severity of symptoms, severity of the disorder, and the desire to have children in the future. Treatment options include medication to control pain, hormonal medications (most commonly birth control) to regulate estrogen production such as Progesterone pills, surgery to remove the growths, or in serious cases hysterectomies (removal of the uterus and potentially the ovaries and fallopian tubes as well).
What to do if you think you may have endometriosis:
The first thing to do is not to worry! Educate yourself as much as possible so that you can ask informed questions and make the best decision for yourself after consulting your doctor.
And, don’t be embarrassed. Your body’s health and your vagina’s health are essential components of your overall mental health. Women who suffer from endometriosis complications can often feel depressed. They may also miss work, school or social engagements due to their pain. Before you can feel like your fabulous, fierce self again, you have to take care of yourself. To keep yourself healthy exercise often, limit your stress, and eat healthy. To keep your vagina healthy, use organic hygiene products such as those produced by Maxim to ensure you do not augment the risk factors of endometriosis by increased chemical sensitivity or exposure to dioxin. Get regular gynecological checkups and ask if anything feels wrong.
If you think you may have endometriosis, schedule an appointment with your gynecologist/ OBGYN. There are several ways in which doctors can examine your condition including pelvic exams, transvaginal ultrasounds, or in complicated cases – a laparoscopy.
For more details on these procedures or if you have any other general questions, please look at the links below.
http://www.womenshealth.gov/publications/our-publications/fact-sheet/endometriosis.cfm
http://www.ncbi.nlm.nih.gov/pubmedhealth/PMH0001913/
http://www.mayoclinic.com/health/endometriosis/DS00289
http://www.endometriosisassn.org/index.html
http://kidshealth.org/teen/sexual_health/girls/endometriosis.html#